News, Information, Research
Meeting for American Society of Clinical Oncology
Chicago, IL : May 31st– June 4 2019
The Metaplastic Breast Cancer Global Alliance was excited to qualify for an ASCO-Sponsored Patient Advocacy Booth this past May 31st through June 4th, 2019. This annual meeting of the American Society of Clinical Oncology provides nonprofit patient organizations the opportunity to meet, interact and exchange information with approximately 40,000 meeting attendees from all over the globe.
British Columbia Canada-- 0
Prince Edward Island, Canada-- 0
Northwest Territories Canada--0
British Columbia Canada--0
Northern Territory Australia--0
New South Wales Australia--2
Scotland, United Kingdom --
Northern Ireland, United Kingdom
Wales, United Kingdom -- 1
England, United Kingdom -- 17
We were able to share our Diagnosed Member Map at our Booth from a LapTop.
Members, Family and Friends
We were very fortunate to have ten diagnosed members, family and friends attend this valuable conference and assist our busy booth. We were thrilled with the welcome we received from doctors all over the world who were surprised to see a patient advocacy group representing MpBC! We shared information with many doctors and even made a short video with a doctor from Brazil so that she could provide better support to her patients!
“Raising Global Awareness and Supporting Research for Metaplastic Breast Cancer”
Continued Need for Research
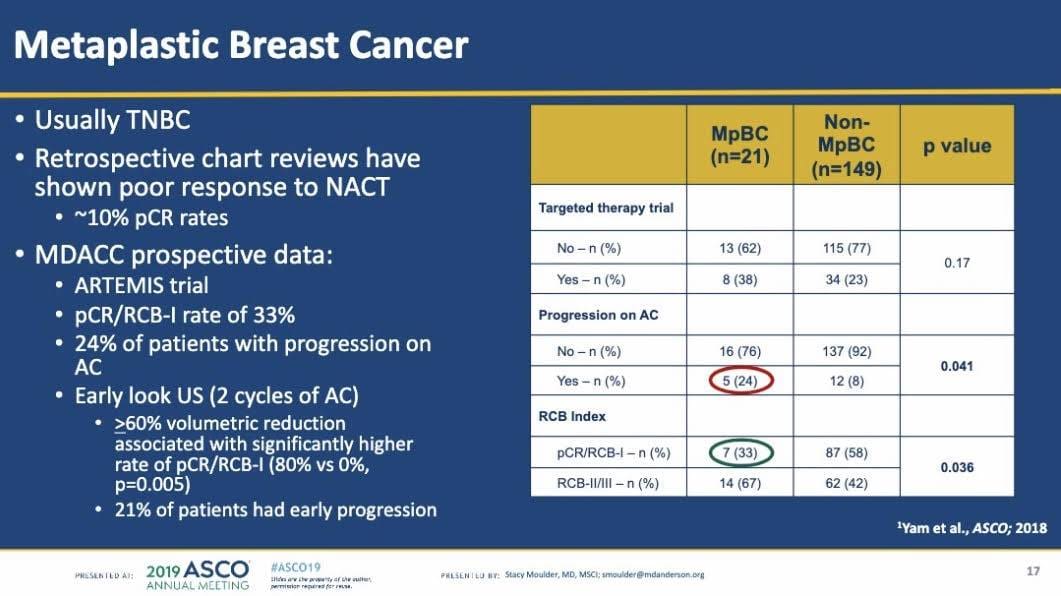
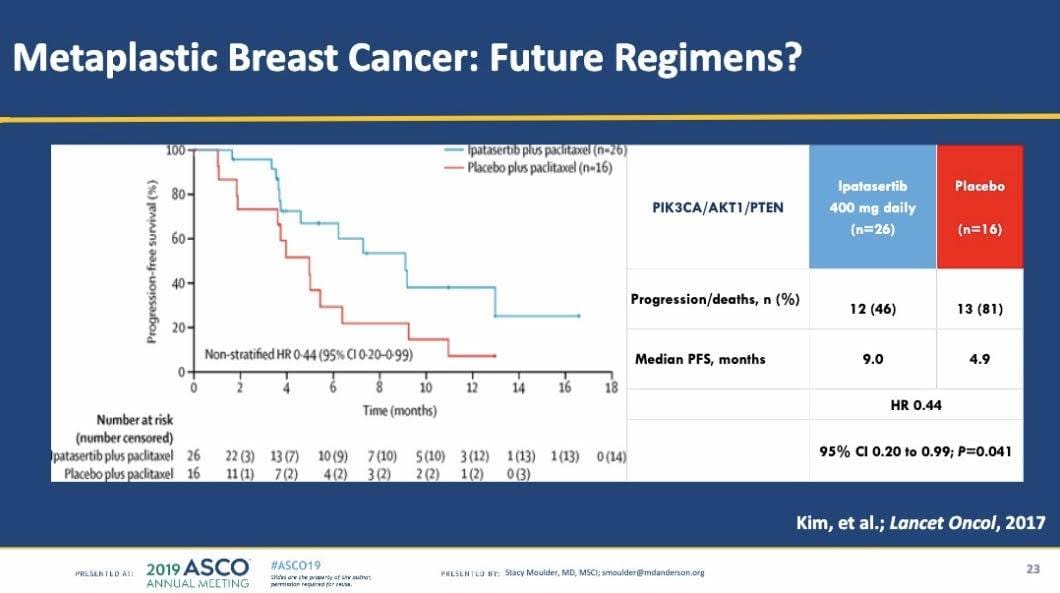
The week was capped off by an early-morning session on Monday the last day of the conference, delivered by Dr. Stacey Moulder, that highlighted Metaplastic Breast Cancer and the need for research.
ASCO is the largest venue for sharing cutting edge scientific and educational developments in oncology and we were very proud of all our efforts and how we represented our rare community.
Meeting with Dr. Moulder at our Booth
Other Patient Advocates We Met
Ian Still Sporting Our Shirt!
Best Memories and Takeaways from ASCO 2019!
Susan D. Oran– “For me, the highlight was hearing Metaplastic Breast Cancer discussed in a session attended by hundreds of doctors at 8am and meeting with Dr. Moulder again. Eating dip-n-dots with my oncologist Dr. Michael Nissenblatt and meeting all of you wonderful people and seeing how we were able to ban together towards our common goals so easily!”
Nancy McCormack Buschener– “Meeting all of you and your amazing doctors. I learned so much! Oh and the cake building!”
Sue McCaldon– “For me it was meeting you all and having the opportunity to go into sessions to learn so much. Also, seeing my doctor and finding my drug trial poster and talking to the research people in the drug company.”
Dr. Janku stopped by to say Hi!
Jim Harvey Sy– “Best part was meeting you guys and learning that there is so much out there focused on finding a cure for cancer”
Casie Friedrich- “For me it was seeing oncologists and other oncology professionals from all around the world looking to us for information to better help their patients! And the Lattes with your face on them!”
Stephanie Oran– “Hearing Dr. Moulder say that social media has provided a way for doctors to meet patient advocacy groups (like us!) Oh and all the free snacks!”
Laura Houmes– “My first takeaway is WOW! I am completely exhausted but was worth all our combined efforts. I can’t say there was any “best” part of our ASCO gathering. The whole event was a blessing to me and more than I could have imagined. Metaplastic breast cancer brought us all together and we all are trying to make a difference. I believe we made all who have donated to our nonprofit proud!”
Finally, just some images from our time at a local historical, 1800s haunted AirBnB!

Information, follow up, News

MpBC Global Alliance, Inc. Recommendations
Metaplastic Breast Cancer is a uniquely complicated, rare breast cancer that to this date is not well understood. Because of higher than normal incidence of metastatic disease in metaplastic breast cancer, follow up monitoring and scanning, either during neoadjuvant therapy or during and after initial treatment, can be critical. Plans for monitoring and scanning should be discussed with a patient and their treating physician early in their treatment plan. Based on surveys of our members, early detection of metastases has resulted in early adoption of additional therapies and has led to long-term survival and NED.
Referencing the ACS/ASCO April 2015 Breast Cancer Survivorship Care Guidelines, diagnosed patients may focus on the Guideline Disclaimer Section. This publication specifically states:
- “The Information herein should not be relied on as being complete or accurate, nor should it be considered as inclusive of all proper treatments of methods of care or as a statement of the standard of care. With the rapid development of scientific knowledge, new evidence may emerge between the time information is developed and when it is published or read.”
The following is also stated:
- “This information does not mandate any particular course of medical care. Furthermore, the information is not intended to substitute for the independent professional judgment of the treating provider, as the information does not account for individual variation among patients.”
The Metaplastic Breast Cancer Global Alliance polled 30 Stage 4 diagnosed members in October 2018. 26 of the 30 reported metastatic disease within 18 months following initial treatments.
Conclusion: Based on the published guidelines and our members’ experiences, patients with metaplastic breast cancer should work with their physicians to establish an aggressive scanning protocol during and after treatment. Physicians should evaluate these patients’ need for careful watching, especially during the first 2 years after treatment, and work with insurance providers to meet these patients’ needs.

Information, News
14 Ways to Advocate for Yourself as a Metaplastic Breast Cancer Patient
 As a patient with a rare disease, it is crucial to take charge of your care
As a patient with a rare disease, it is crucial to take charge of your care
You, as a patient with Metaplastic Breast Cancer (MpBC), have been given life-changing news. Suddenly your world is turned upside down. Your days are filled with nonstop doctor’s appointments, scans, radiation, bloodwork, and chemotherapy. It can all become very overwhelming, and it’s often difficult to keep up with all the new information you are being given.
It Takes Work
My mother — a Metaplastic patient herself — learned that she had to become her own advocate. Once she found out she had MpBC, she researched it endlessly online. She wrote down questions she had and brought them to her appointments. She bought a binder and organized all her reports. She did her best to understand how to read lab results. She was able to get valuable information from the members of the Facebook support groups she joined. She went through the usual surgery, chemotherapy, and radiation therapy.
Left with No Options
After a lung resection of the initial nodule, my mother’s cancer reoccurred. Clinical trials were then her best option. She ended up going on a clinical trial that kept her stable. The side-effects affected her liver so bad that she was pulled out of the trial.
Left with no options, she told her story on Facebook and did a lot of online research. Because of her efforts, she ended up finding a clinical trial at MD Anderson Cancer Center in Houston, Texas. The trial ultimately worked and she is still with us today — 5 years later. This is why being a proactive patient is so important.
Get the Upper Hand
Metaplastic Breast Cancer is very fast growing. It is also very rare, accounting for less than one percent of all breast cancers [1]. Because it’s so rare, there aren’t many oncologists that are familiar with exactly how to treat it. In fact, there isn’t even a specific standard-of-care treatment for this type of cancer. It is treated the same as invasive breast cancer and triple-negative breast cancer [2].
One thing we’ve learned is staying ahead of disease progression gives patients the upper hand. You must have your next plan-of-action in your back pocket. This way, you can immediately take the next steps.
You Are Also a Member of Your Care Team
I cannot emphasize this enough. You are a vital member of your care team. As a patient diagnosed with a rare type of cancer, it is absolutely crucial that you stay on top of your care. Yes, it’s scary — and stressful — but your future depends on you taking an active role in your health. Below are some helpful tips that can help give you a jump-start on being your own patient advocate:
- Keep a binder so that you can organize all test results, imaging, pathology reports, and visit notes in. It’s important that you ask for copies of these so you can hand-deliver them to other physicians that are on your care team. It is also helpful to keep for your own reference.
- Use the calendar on your phone and set reminders for your appointments — or a physical calendar that you can handwrite them in.
- Have a friend or family member with you taking notes while you talk with the doctor. It’s good to have another set of ears and emotional support.
Speaking of support…
- Join a support group. Facebook is a great way to connect with many support groups. There are some specific to MpBC — the MpBC Global Alliance Facebook group is a great place to start. These groups not only supply emotional support, but also valuable information on new research, clinical trials, and ways to handle side-effects of cancer treatment. In-person support groups and seeing a therapist are also great options.
- Focus on taking care of yourself. This is a good time to reflect back on your past and examine any bad health habits. Not saying they caused this cancer, but you need to strengthen your body. You need to stay as strong as possible mentally and physically during cancer treatments. Seeing a nutritionist can support this effort.
- Set an alarm or reminder on your phone to take your medications.
- Make sure your oncologist is familiar with MpBC. Being that this is a very rare type of cancer, it is important to make sure your cancer care team is familiar with it or has treated patients with it in the past.
- Get a second opinion. It’s absolutely OK to get a second opinion. Especially when you’re diagnosed with a rare disease. Don’t worry about offending your doctor. Any good practitioner would respect your right to one. This is a time where you should consider all your options, and have a reassurance that you have the right treatment plan for you.
- Schedule a port placement. Ask your oncologist about getting a port placed. This will make it easier on your veins and give better access when you are having frequent blood draws and IV medications administered.
- Discuss having genomic testing done on your tumor with your oncologist. This will help your doctor individualize your treatment. There’s a list of companies that do this listed here.
- Have regular scans to track disease progression. Get a plan in place with your oncologist to have regular scans done to track the status of your cancer.
- Develop an understanding of the terminology. You’re probably asking, “Why should I need to know that?” Well, it’ll help you understand your diagnosis better and in decision-making. This is part of being a proactive patient.
- Know the possible side-effects of your treatment. This way you know what to look out for ahead of time and how you can treat them.
- Write down questions that pop into your head during the day and bring that list in with you to your appointment. Having your questions answered will give you some peace of mind.
Communication Is Key
Express to your physicians and care team how you feel. It’s true when they say that you know your body better than anyone else. Is something bothering you? Are you feeling depressed? Is there a new pain that you’ve been experiencing? If something doesn’t feel right, let your doctor know! Communication is key in healthcare.
If there is anything that your physician is talking to you about you don’t understand, ask them to repeat it in a different way. All this ensures that you are getting the best care. Patients who play an active role in their care usually have better outcomes when compared to patients who play a passive role [3]. So, I hope these tips help involve you in your care and take charge of your health today.
Casie Friedrich, PA-C